As Africa commemorates World Malaria Day 2026, a stark reality persists: malaria remains one of the continent’s most devastating yet preventable public health challenges. The scale of its impact is enormous. In 2024 alone, Africa recorded an estimated 270.8 million malaria cases and close to 600,000 deaths. These figures represent the overwhelming majority of the global burden, with nearly all cases and deaths occurring on the continent. The disease continues to disproportionately affect the most vulnerable groups—especially children under the age of five and pregnant women—highlighting deep inequities in health outcomes and access to care.
Malaria is far more than a medical issue. Its consequences ripple through every aspect of development. By weakening the health and productivity of populations, it reduces workforce capacity, strains healthcare systems, and entrenches poverty. Families face lost income due to illness, while governments bear the economic cost of treatment and prevention efforts. In this way, malaria acts as a significant barrier to Africa’s broader development ambitions, including the goals outlined in Agenda 2063 and the pursuit of universal health coverage.
Over the last two decades, there has been meaningful progress in the fight against malaria. The widespread distribution of insecticide-treated mosquito nets, the use of indoor residual spraying, and improvements in diagnostic testing and treatment have collectively saved millions of lives. The adoption of artemisinin-based combination therapies, along with seasonal malaria chemoprevention and the introduction of malaria vaccines in some regions, has further strengthened control efforts. Community-based healthcare delivery systems have also played a vital role in extending services to underserved populations.
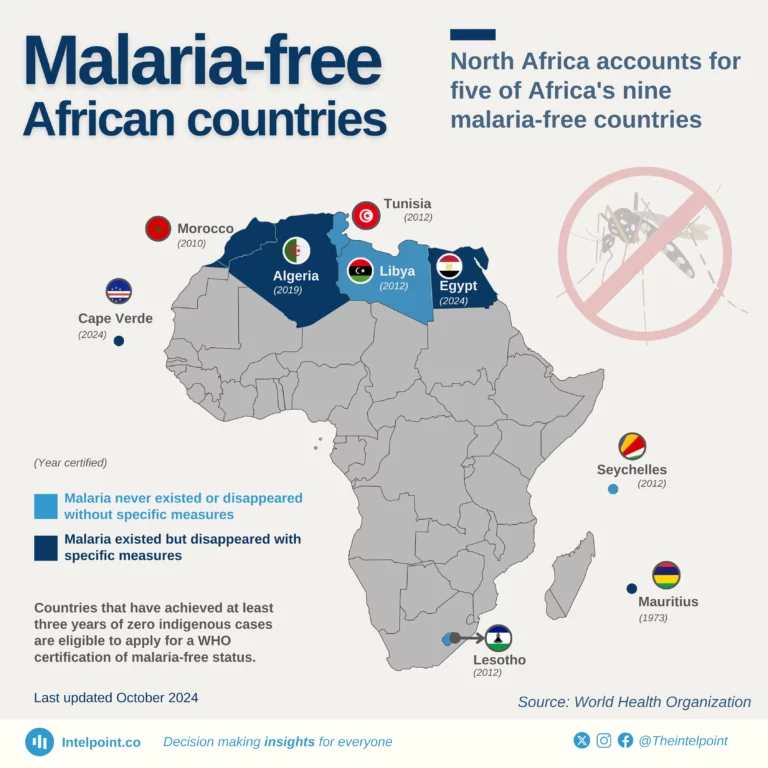
Encouragingly, a few African countries have achieved malaria-free certification, demonstrating that elimination is possible. Others have successfully reduced transmission rates to very low levels through strong surveillance systems, targeted interventions, and sustained political will. These success stories underscore an important lesson: malaria outcomes are not predetermined by geography or climate. Rather, they are shaped by the quality of leadership, the effectiveness of implementation, the level of accountability, and the consistency of investment.
Despite these gains, progress remains fragile and uneven. Recent data suggest that malaria cases are rising again in several parts of the continent, signaling a troubling reversal of earlier achievements. The goal of eliminating malaria by 2030 is still within reach, but it is increasingly clear that current efforts are insufficient. New and evolving challenges are complicating the fight.
One major concern is the emergence of partial resistance to artemisinin, the cornerstone of modern malaria treatment. This development threatens to undermine the effectiveness of first-line therapies, making infections harder to treat and control. At the same time, resistance to insecticides is reducing the impact of key vector control tools such as treated bed nets and indoor spraying. These challenges demand continuous monitoring and the adoption of new, more effective technologies.
Climate change is adding another layer of complexity. Shifting weather patterns are altering mosquito habitats, extending transmission seasons, and increasing the frequency of extreme events such as floods and droughts. These environmental changes create conditions that facilitate the spread of malaria into new areas and intensify outbreaks in existing ones. Additionally, humanitarian crises, population displacement, and gaps in funding are further straining already fragile health systems.
Taken together, these factors reveal a critical weakness in the current response to malaria. The issue is no longer simply about the availability of tools and commodities. Instead, the focus must shift to the strength and efficiency of the systems that deliver these interventions. The key question is whether countries can provide prevention, diagnosis, treatment, and surveillance services quickly, accurately, and equitably enough to keep pace with the evolving nature of the disease.
This is why malaria should now be seen as a central test of Africa’s broader health security and sovereignty. A continent cannot claim true health independence while a preventable and treatable disease continues to claim hundreds of thousands of lives each year. Strengthening malaria control is therefore inseparable from building resilient public health institutions. It requires robust primary healthcare systems, reliable laboratory networks, effective disease surveillance, and secure supply chains that ensure essential commodities reach even the most remote communities.
To accelerate progress toward elimination, several strategic actions are essential.
First, strong political commitment at the highest levels is crucial. Leadership must go beyond declarations and translate into sustained action, adequate funding, and clear accountability. Governments need to take ownership of malaria control efforts, aligning national strategies with local realities and ensuring consistent implementation.
Second, better evidence is needed to understand why progress has stalled in some areas and how emerging threats are shaping the disease landscape. This includes studying the spread of drug and insecticide resistance, the effects of climate variability, and the impact of conflict and instability on healthcare delivery. Data should be collected and analyzed in a coordinated manner, combining routine health information with research and advanced analytics. Most importantly, this knowledge must be translated into practical strategies that can be adapted to different contexts across countries and regions.
Third, improved coordination is vital. Fragmented efforts often lead to inefficiencies and missed opportunities. A unified approach—where countries and partners work within a shared framework—can enhance accountability, streamline decision-making, and ensure resources are used effectively. Strengthening collaboration across borders is particularly important, as malaria does not respect national boundaries.
Fourth, community-based healthcare systems must be at the heart of the response. Expanding the network of community health workers can significantly improve access to prevention and treatment services. When properly trained and supported, these workers can deliver care at the grassroots level, monitor disease trends, and provide critical health education. Integrating malaria services with other health programs—such as maternal and child health, nutrition, immunization, and sanitation—can further enhance efficiency and impact.
Finally, ensuring reliable access to essential malaria commodities is indispensable. This includes not only distributing existing tools but also investing in local manufacturing to reduce dependence on external suppliers. Building strong procurement systems and creating sustainable markets for these products can help guarantee consistent availability and affordability.
Ultimately, eliminating malaria by 2030 will require more than ambition. It demands coordinated action, sustained investment, and unwavering commitment. Africa has reached a pivotal moment where malaria can no longer be treated as routine business. The scale and persistence of the problem call for urgency, innovation, and decisive leadership.
The path forward is clear. By strengthening health systems, empowering communities, embracing data-driven strategies, and fostering collaboration, Africa can turn the tide against malaria. The disease has taken a heavy toll on the continent for far too long. With the right actions, it is possible not only to control malaria but to end it entirely.
The time to act is now.




