Peptic ulcers—commonly referred to as stomach ulcers—are open sores that develop in the lining of the stomach or the upper part of the small intestine. When they occur in the stomach, they are known as gastric ulcers; when they appear in the first part of the small intestine (the duodenum), they are called duodenal ulcers. Although the condition can be painful and sometimes serious, most people recover fully with appropriate treatment.
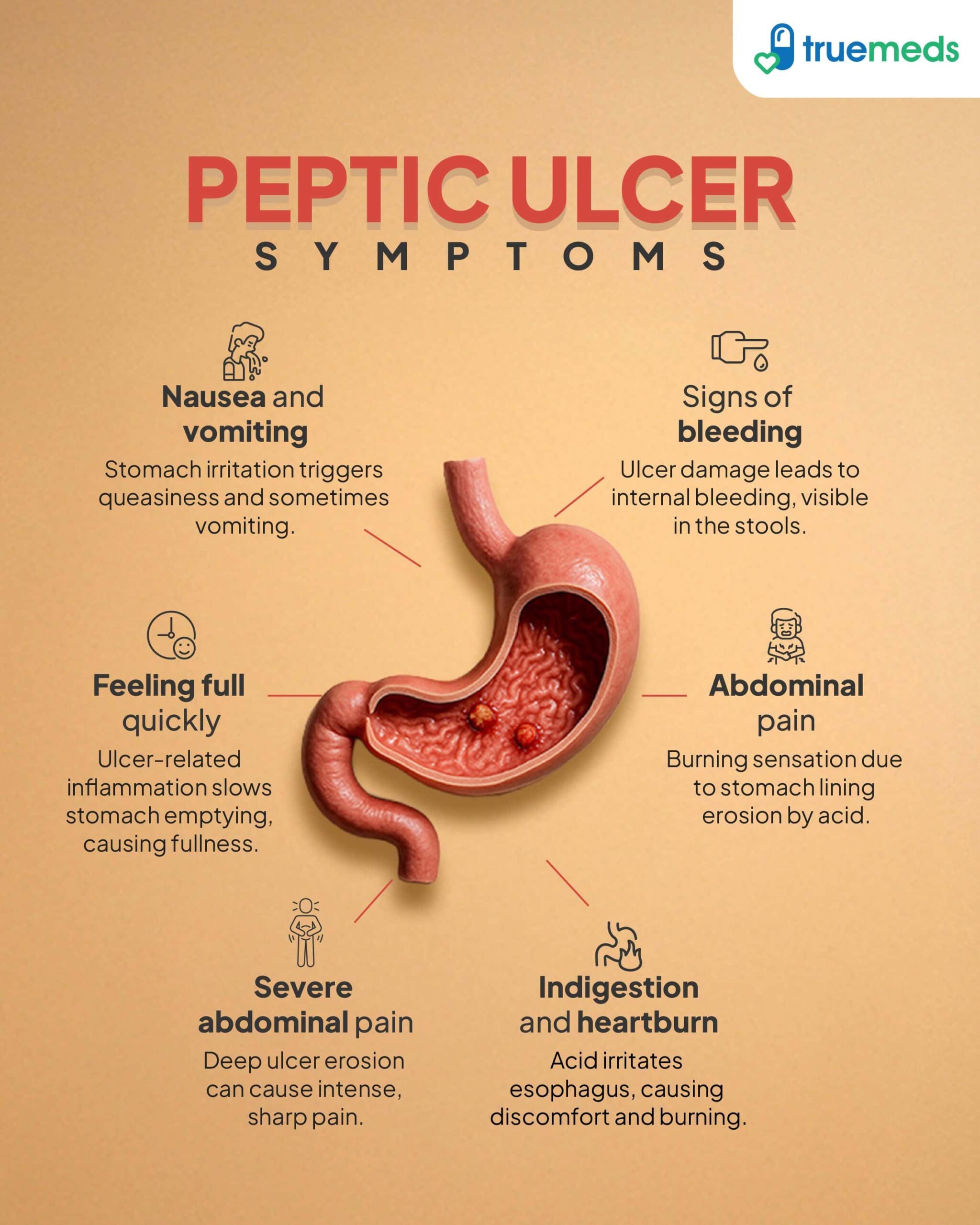
The most common symptom of a peptic ulcer is abdominal pain. This pain is typically felt in the upper part of the abdomen and is often described as a dull, burning sensation. For some individuals, the discomfort worsens between meals or during the night, while others may notice increased pain shortly after eating. In addition to pain, people may experience bloating, belching, heartburn, indigestion, nausea, or a feeling of fullness after eating only a small amount of food.
However, not everyone with a peptic ulcer experiences obvious symptoms. In some cases, complications may be the first sign of a problem. Bleeding ulcers can cause vomiting of bright red blood or material that looks like coffee grounds. Stools may become black, sticky, tarry, or contain visible blood. Significant blood loss can also lead to dizziness, fainting, fatigue, or iron deficiency anaemia. Severe abdominal pain, especially if the abdomen becomes tender to touch, may signal a more serious complication such as a perforation—a hole in the stomach or intestinal wall—which requires urgent medical attention.
Peptic ulcers develop when the protective lining of the stomach or small intestine is damaged, allowing digestive acid to erode the tissue beneath. Normally, a layer of mucus shields the digestive tract from stomach acid. When this balance is disrupted—either by excess acid or reduced protective mucus—an ulcer can form.
Two primary causes account for most peptic ulcers. The first is infection with Helicobacter pylori (H. pylori), a type of bacteria that lives in the stomach lining. While many people carry this bacterium without symptoms, it can trigger inflammation of the stomach’s inner layer, increasing vulnerability to ulcer formation. H. pylori may spread through close personal contact or contaminated food and water.
The second major cause is the regular use of nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, naproxen, and aspirin. These medications can irritate and inflame the stomach lining, especially when taken frequently, at high doses, or over a long period. The risk is greater in people over 60, those who have previously had ulcers, and individuals who combine NSAIDs with other medications such as steroids, blood thinners, certain antidepressants, or drugs used to treat osteoporosis. It is important to note that acetaminophen (paracetamol) does not belong to the NSAID group and does not typically carry the same ulcer risk.
Contrary to popular belief, stress and spicy foods do not directly cause peptic ulcers. However, they can aggravate symptoms and make discomfort more noticeable. Smoking and excessive alcohol consumption can also worsen ulcers and delay healing. Smoking, in particular, increases ulcer risk among people infected with H. pylori and makes recurrence more likely.
Diagnosis usually begins with a medical evaluation. A healthcare provider may ask about symptoms, review medications, and examine the abdomen. Tests to detect H. pylori can include a breath test, blood test, or stool test. In some cases, especially when symptoms are severe, persistent, or concerning, a gastroscopy (also known as an endoscopy) may be performed. This procedure involves passing a thin, flexible tube with a camera through the mouth into the stomach to directly view the lining and check for ulcers or other abnormalities.
Treatment depends on the underlying cause. If H. pylori infection is present, a combination of antibiotics is prescribed to eliminate the bacteria. In addition, medications known as proton pump inhibitors (PPIs) or other acid-reducing drugs are used to decrease stomach acid and allow the ulcer to heal. When NSAIDs are responsible, a doctor may recommend stopping the medication, lowering the dose, or switching to an alternative. In some cases, protective medications are added to reduce further irritation. Treatment may last from one week to several weeks, and follow-up testing may be needed to confirm that the infection has cleared and the ulcer has healed.
Without treatment, peptic ulcers can lead to serious complications. These include internal bleeding, which may develop gradually or occur suddenly and severely; perforation of the stomach or intestinal wall, leading to infection of the abdominal cavity (peritonitis); and obstruction, where swelling or scarring blocks food from passing through the digestive tract, causing vomiting, early fullness, and weight loss. Long-standing H. pylori infection is also associated with an increased risk of stomach cancer.
There are practical steps individuals can take to reduce their risk or prevent recurrence. Using NSAIDs cautiously—taking them with meals, at the lowest effective dose, and only when necessary—can help protect the stomach. Avoiding smoking and limiting alcohol intake are strongly recommended. Eating smaller meals, avoiding foods that trigger symptoms, maintaining a healthy weight, and managing stress can also ease discomfort. Anyone experiencing persistent indigestion, recurring abdominal pain, unexplained weight loss, difficulty swallowing, or signs of bleeding should seek medical care promptly.
Peptic ulcers are common but treatable. Early recognition of symptoms, appropriate medical evaluation, and adherence to treatment greatly reduce the risk of complications and support full recovery.